Did you know many people in First Nations communities wait weeks or even months to see a doctor or nurse? In some places, the nearest clinic is hours away. That means long trips, missed checkups, and health problems that get worse over time. It’s a tough gap to live with. Without better access to care, communities face more sickness, more costs, and more stress on families. The hope is simple: stronger and healthier First Nations communities where care is close, safe, and dignified. The big question is how to make that happen.
At MoveMobility, we’ve been helping communities find answers for over 20 years. We’ve built more than 150 mobile medical units that travel across Canada, designed around what each community needs most. Every vehicle meets high safety standards like Ford QVM, Stellantis QPro, and Canada’s National Safety Mark. Communities like Liard First Nation have worked with us because we take time to listen before we build. We know we’re not the only company out there, but we share what we’ve learned so you can make the best choice for your people.
In this article, you’ll learn:
- The healthcare gaps facing First Nations communities
- How Mobile Clinic Vans can help close those gaps
- How these vans support stronger, healthier communities
What are the biggest healthcare gaps that First Nations communities face?
Healthcare access is uneven across Canada. For many First Nations communities, the gaps are wide and deeply felt. These gaps affect daily life, health outcomes, and the strength of communities. Let’s take a look at some of the big gaps they face.
1. Long travel times
Many First Nation communities in Ontario, Manitoba, and BC are hours from the nearest hospital. Some rely on small nursing stations with limited services.
- Dialysis patients: People often travel from northern Ontario or Manitoba to larger centers like Winnipeg or Thunder Bay, three times a week for treatment.
- Specialist care: A cancer patient in a remote First Nation community in BC may need costly flights south for treatment.
This travel is exhausting, expensive, and disconnects people from family and culture.
2. Limited health staff
Even when a clinic is nearby, it often doesn’t have enough staff. Many First Nations communities rely on fly-in doctors or nurses who come only a few days each month.
- Everyday care: A child with asthma in a First Nation community in Alberta may wait weeks for follow-up.
- Simple conditions: Skin infections or minor wounds can turn serious when early care isn’t available.
3. High rates of chronic illness
Chronic diseases affect First Nations communities more heavily than the rest of Canada.
- Diabetes: Indigenous adults are nearly four times more likely to live with diabetes than non-Indigenous adults (Government of Canada).
- Kidney disease: Higher rates mean more people needing regular dialysis, which is hard when services are far away.
Without consistent care, these illnesses worsen and lead to higher costs and stress.
4. Mental health and addiction challenges
Mental health services are also scarce. Many First Nation communities in Manitoba and Nova Scotia face high rates of depression, suicide, and substance use.
- Counselling access: Young people may wait months to see a counsellor, or have no one available at all.
- Short-term fixes: Fly-in services don’t always provide the ongoing support people need.
5. Emergency delays
Emergencies are harder to handle when care is far away.
- Response times: Some First Nation communities in New Brunswick or northern Alberta don’t have an ambulance based nearby.
- Weather barriers: In winter, icy roads or storms in northern Manitoba can delay urgent care for hours.
These gaps leave First Nations communities carrying a heavier health burden than most Canadians. Without action, the cycle continues: More sickness, more travel, and more stress.
Next, we’ll look at how Mobile Clinic Vans give communities new ways to close these gaps and bring care closer to home.
How do Mobile Clinic Vans close First Nations healthcare gaps?
You’ve now seen some of the gaps First Nations communities deal with: Long travel, few staff, chronic illness, mental health issues, and emergencies that are hard to handle. Mobile Clinic Vans are efficient tools to help close those gaps in First Nations communities. You can use them to bring care to people instead of making people chase care.
Here’s a look at how they can do that.
1. Bringing care close to home
Problem: Many First Nation communities have to travel hours for anything beyond basic care. Even routine checkups or follow-ups are far away.
How the Mobile Clinic Van helps:
- The MC Model is built so that it becomes a doctor’s office on wheels. It travels into remote areas so people don’t have to drive long hours.
- Because it is mobile, it shows up at communities, homes, or nearby gathering places. It makes access possible for those who cannot leave easily.
Example: A First Nation community in northern BC that doesn’t have a clinic may use a Mobile Clinic Van to deliver routine health checks, diabetes monitoring, even family wellness services, saving families from costly travel or leaving the community.
2. Handling chronic illness earlier
Problem: Diseases like diabetes or kidney issues grow worse when treatment isn’t ongoing. Without early detection or treatment, these become bigger emergencies.
How the Mobile Clinic Van helps:
- Your community or organization can use it to give basic primary healthcare, diagnostic tools, and ongoing monitoring. MC vans include exam beds, office work space, and refrigerated medicine storage.
- Staff can use the van to give treatment before problems become emergencies, catching issues early prevents hospital stays and health decline.
3. Reducing the stress of travel and missed appointments
Problem: Travel costs, long waits, and missed work or school add up. For many, going to town for healthcare means losing a day or more, time with family, or dealing with bad weather.
How the Mobile Clinic Van helps:
- Your community can use it to give families care without long, expensive travel.
- Your organization can use it to give people fewer disruptions to daily life, so they don’t have to miss work, school, or cultural events.
Example: A community in Manitoba with poor road access in winter may schedule the van to visit monthly, providing vaccinations, prenatal checks, or chronic disease care, reducing missed care and helping people feel cared for locally.
4. Meeting mental health, addiction, and culturally safe care needs
Problem: Mental health and addiction supports are very limited in many First Nations communities. Services may feel unsafe, disconnected, or not culturally relevant.
How the Mobile Clinic Van helps:
- Your organization can use the van to provide a private, welcoming space for counselling or peer support so people feel safer.
- Your community can use it to give culturally safe programs like mental health counselling, sexual health education, and addiction services where people already gather.
The Mobile Counselling Van is also a useful tool for providing mental health counselling services.
5. Flexibility and customization for First Nations communities
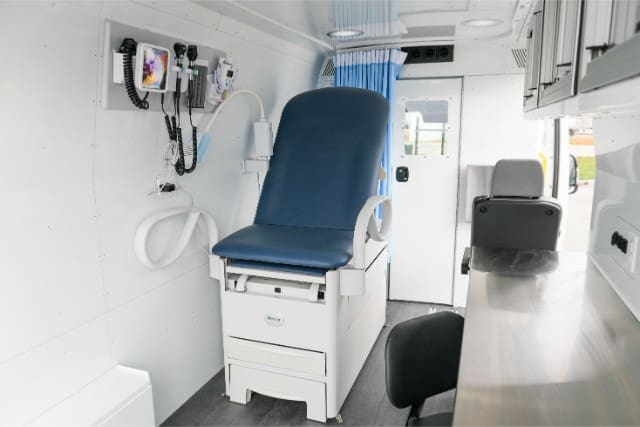
Every First Nation community is different. Mobile Clinic Vans let you build what your community needs.
Key features of the MC Model van:
- Custom layouts: Your community can use it to give space for an exam bed, sink, fridge, or storage for wellness supplies.
- Comfortable environment: Your organization can use it to give care in a warm, safe space with good heating, cooling, and lighting.
- Accessibility features: Your community can use it to give safe entry with ramps, wide doors, and layouts for those using mobility aids.
6. Private, non-emergency services for ongoing support
Problem: Many communities only get clinics for emergencies or fly-in days. They lack consistency and privacy for ongoing non-emergency healthcare.
How the Mobile Clinic Van helps:
- Your organization can use it to give a private space for non-emergency care like lab work, prenatal visits, or chronic illness follow-up.
- Your community can use it to give educational sessions and wellness programs in a more comfortable setting.
7. Economic and health fairness impact
Problem: Gaps in care also create bigger costs: More severe disease, more hospital stays, and more burden on families and the health system.
How the Mobile Clinic Van helps:
- Your community can use it to give early care that prevents ER visits.
- Your organization can use it to give prevention programs that save money and improve health over time.
How can Mobile Clinic Vans support youth and Elders in First Nations Communities?
In many First Nations communities, youth and Elders are the heart of the community. But both often face big gaps in healthcare. Youth need safe places to talk about their health and feelings. Elders need regular care for things like diabetes, heart problems, or arthritis. Too often, those services are far away or not available at all.
What are the challenges for youth?
In some First Nation communities in BC or Ontario, youth may have to travel hours to see a counsellor. Talking about mental health, substance use, or sexual health in a busy hospital outside the community can feel scary or uncomfortable.
A Mobile Clinic Van can help your youth by:
- Safe space: Your community can use the van to give young people a private and welcoming place to talk.
- On-site programs: The van can bring workshops on nutrition for better health, mental wellness, or health right to your school or youth center.
- Consistency: When the van shows up regularly, youth begin to trust the service and feel comfortable reaching out.
Example: A community in BC could have the van visit the school once a month to offer checkups and private counseling sessions.
What are the needs of Elders?
Elders carry wisdom and guide younger generations. But they also face some of the toughest health issues. In rural First Nation communities in Manitoba or Alberta, Elders may need dialysis, diabetes care, or wound treatment. Getting to a hospital in a city can mean long, tiring trips, sometimes in dangerous winter weather.
A Mobile Clinic Van can help your Elders by:
- Accessibility: Vans can have ramps and wide doors so Elders with walkers or wheelchairs feel safe.
- Primary care: Your team can use the van to give checkups, diabetes support, or blood pressure checks right in the community.
- Reduced travel: When the van comes to them, Elders don’t have to leave their homes as often.
Example: In Manitoba, a van could visit nearby First Nations on a weekly schedule so Elders don’t need to travel into Winnipeg for routine care.
When youth and Elders both have support, the entire community is stronger. Youth feel seen and valued, and elders stay healthy and connected so they can keep sharing their knowledge.
Your Mobile Clinic Van can even serve both in the same day:
- Morning visits: Elders can get wellness checks and support for chronic health issues.
- Afternoon visits: Youth can take part in workshops or counseling sessions.
A Mobile Clinic Van is a bridge between generations. It helps your community care for its future and honor its past at the same time.
Ready to build a healthier First Nations community with a Mobile Clinic Van?
You came to this article because your community is searching for ways to close the healthcare gap and create stronger futures. You’ve seen the barriers, and you want solutions that bring care closer to home.
Here’s what you learned in this article:
- The challenge: First Nations communities often face long travel times and limited access to care.
- The solution: Mobile Clinic Vans can deliver health services directly to your people.
- The impact: Better access builds dignity, stronger health, and trust within your community.
At MoveMobility, we’ve seen how the right vehicle can change lives: From making it easier for Elders to access care to helping youth feel supported and everyone in between. We believe mobile care isn’t a luxury; it’s a necessity, and we’re proud to be a partner in that journey.
Mobile Clinic Vans give First Nations communities the power to decide how care is delivered. They help protect health, strengthen connections, and open new doors to wellness. If you’d like to learn more, click the button below to talk with a mobility expert.
If you’re not ready to chat yet, here are three other articles you can read to take the next step:
- What are the different uses of mobile clinics? Learn about some of the different ways you can use your Mobile Clinic Van
- How Much Does a Mobile Medical Van Cost in 2025?: Understand the investment so you can plan your project with clarity.





